Prof. Dr. J. Morschhäuser
Research
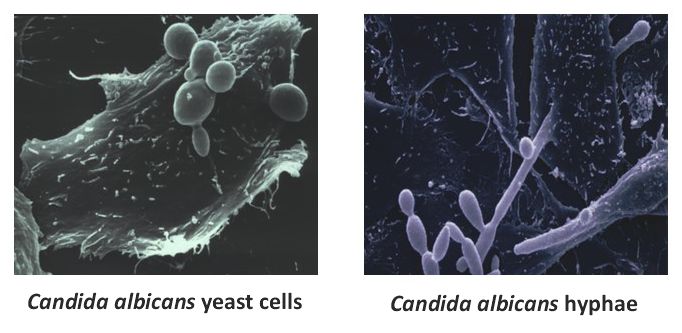
Our group studies the yeast Candida albicans, which is a member of the microbiota of the gastrointestinal and genitourinary tracts in most healthy persons. Especially in immunocompromised patients, this normally harmless fungus can become a pathogen and cause superficial infections of the mucosa and skin as well as life-threatening systemic infections after dissemination via the bloodstream. Adaptation of the gene expression pattern to altered environmental conditions in new host niches, induction of developmental programs that involve changes in its morphology, and genomic alterations that result in the acquisition of novel phenotypic traits all contribute to the success of C. albicans as a commensal and pathogen in the human host and are topics of our research projects.
Staib P, Kretschmar M, Nichterlein T, Hof H, Morschhäuser J (2000) Differential activation of a Candida albicans virulence gene family during infection.
Proc. Natl. Acad. Sci. USA 97:6102-6107.
Morschhäuser J, Barker KS, Liu TT, Blaß-Warmuth J, Homayouni R, Rogers PD (2007) The transcription factor Mrr1p controls expression of the MDR1 efflux pump and mediates multidrug resistance in Candida albicans.
PLoS Pathog. 3:e164.
Hampe IAI, Friedman J, Edgerton M, Morschhäuser J (2017) An acquired mechanism of antifungal drug resistance simultaneously enables Candida albicans to escape from intrinsic host defenses.
PLoS Pathog. 13:e1006655.
Popp C, Ramírez-Zavala B, Schwanfelder S, Krüger I, Morschhäuser J (2019) Evolution of fluconazole-resistant Candida albicans strains by drug-induced mating competence and parasexual recombination.
mBio 10:e02740-18.
Ramírez-Zavala B, Krüger I, Dunker C, Jacobsen ID, Morschhäuser J (2022) The protein kinase Ire1 has a Hac1-independent essential role in iron uptake and virulence of Candida albicans.
PLoS Pathog. 18:e1010283.
Prof. Dr. Joachim Morschhäuser

Ines Krüger
![[Translate to Englisch:] [Translate to Englisch:]](/fileadmin/_processed_/8/7/csm_Ines_K_adfd042bc1.jpg)
Dr. Bernardo Ramírez-Zavala
![[Translate to Englisch:] [Translate to Englisch:]](/fileadmin/_processed_/c/8/csm_Bernardo_R_a74e3e22f3.jpg)
Sonja Schwanfelder
![[Translate to Englisch:] [Translate to Englisch:]](/fileadmin/_processed_/7/6/csm_Sonja_S_f1b1166beb.jpg)